|
Pseudogout is a similar type of arthritis resulting from crystal deposition of calcium pyrophosphate (CPP) and is also known as calcium pyrophosphate deposition (CPPD) disease. Comorbidities associated with hyperuricemia include obesity, metabolic syndrome, type 2-diatetes mellitus, hypertension and chronic kidney disease. Non-modifiable risk factors for gout include older age, male gender, post-menopausal women, congenital errors in purine metabolism (i.e., Lesch-Nyhan Syndrome), and African American ethnicity. 1 An acute attack can be precipitated by physiological stressors such as situations causing a relatively rapid rise in uric levels including acute illness, myocardiac infarction, stroke, surgery, rapid volume changes, diuretics, large consumption of alcohol or purine rich foods, and low-dose aspirin can lead to a relatively rapid rise in uric acid levels precipitating an acute gout attack. Uric acid is excreted via the gastrointestinal tract and kidneys, with approximately 65% of uric acid excreted renally. red meats, shellfish, high fructose, liver, and alcohol), uric acid overproduction and/or decreased excretion of uric acid. Hyperuricemia can result from uric acid accumulation, especially with purine rich diet (i.e. However, both monoarticular and polyarticular arthritis is possible with affected joints including ankles, knees, hands, wrist and elbows and thus, sometimes gout is overlooked as the etiology of joint pain.ĭeposition of MSU crystals occur when uric acid levels change rapidly, usually in the setting of hyperuricemia (serum uric acid level greater than 6.9 mg/dL). The classic attack occurs in the first metatarsal phalangeal joint (podagra). Deposition of crystals leads to an acute inflammatory response and this monoarticular synovitis cause severe pain, swelling, redness and tenderness. 
Individuals should consult a qualified health care provider for professional medical advice, diagnosis and treatment of a medical or health condition.Gout is a disease of purine metabolism characterized by acute, subacute, and chronic arthritis, due to deposits of needle shaped monosodium urate (MSU) crystals in joints, tendons, and subcutaneous tissues. This information is provided for general education only. Updated February 2023 by Mohammad Ursani, MD, and reviewed by the American College of Rheumatology Committee on Communications and Marketing. These health care providers guide therapy to improve flexibility, ease joint pain and adapt movements for better function. Rheumatologists may refer some people with CPPD to physical and occupational therapists. See a rheumatologist as soon as symptoms appear to rule out other possible causes and start treatment. Prompt diagnosis and treatment of CPPD may ease symptoms and prevent joint damage. Surgery may be used to repair or replace damaged joints. For severe attacks or chronic inflammation, drugs like methotrexate) or the interleukin beta-1 antagonist anakinra (Kineret) are treatment options. colchicine or low dose NSAIDs can be used to prevent future attacks. The rheumatology provider may drain fluid from the affected joint and inject a corticosteroid. Nonsteroidal anti-inflammatory drugs (NSAIDs) are prescribed to treat joint pain and swelling in an acute CPPD event.There is no treatment to dissolve the crystals. MRI, ultrasound, CT scan or X-ray may show calcium containing deposits in cartilage. Additionally, the rheumatology provider may need to withdraw fluid from a joint to make the diagnosis of CPPD. A rheumatologist diagnoses CPPD based on symptoms and medical tests. Joint cartilage may break down, causing disability. If left untreated, CPPD may lead to severe, painful attacks and chronic joint inflammation. Knees are the joints most commonly affected, but CPPD can other joints. What Are the Signs/Symptoms?ĬPPD symptoms include severe joint pain, warmth and swelling. CPP crystals may also be found in the joints of people with osteoarthritis or gout. Excess iron or calcium, or low magnesium, and an abnormal thyroid gland may be contributing factors. Crystal deposits trigger an inflammatory attack in the joint. People over 60 are more likely to get CPPD, although it may happen at an earlier age. 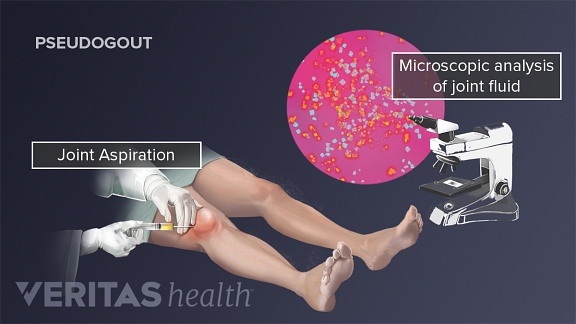
In CPPD, calcium pyrophosphate (CPP) crystals form in the blood and settle in joint cartilage. Calcium pyrophosphate deposition (CPPD)also known as “pseudogout” is a type of arthritis.
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
